Placebo Isn't a Quitting Method

A placebo is not a nicotine dependency recovery method, and it certainly is not the same as quitting cold turkey.
Why care? Because if you've ever tried replacement nicotine, sham placebo studies helped motivate you to waste your money and squander your dreams. Understanding how pharma cheats may help prevent you from being cheated again.
Webster's defines "placebo" as "1. usually pharmacologically inert preparation prescribed more for the mental relief of the patient than for its actual effect on a disorder. 2. an inert or innocuous substance used especially in controlled experiments testing the efficacy of another substance (as a drug)."
Placebos have historically served as the gold standard in clinical research. Study participants are randomized to either the drug being tested or to a placebo look-alike. The objective is to "blind" participants as to the type of treatment they're receiving, so that assignment awareness doesn't affect their response to it.
Falsehood #4: Placebo-controlled clinical trials were blind
While placebo may be the gold standard in most medical research, in smoking cessation it becomes license to steal. The blinding problem is two-fold. Either the expectations of the addict who is experienced in attempting recovery are fulfilled or they suffer.
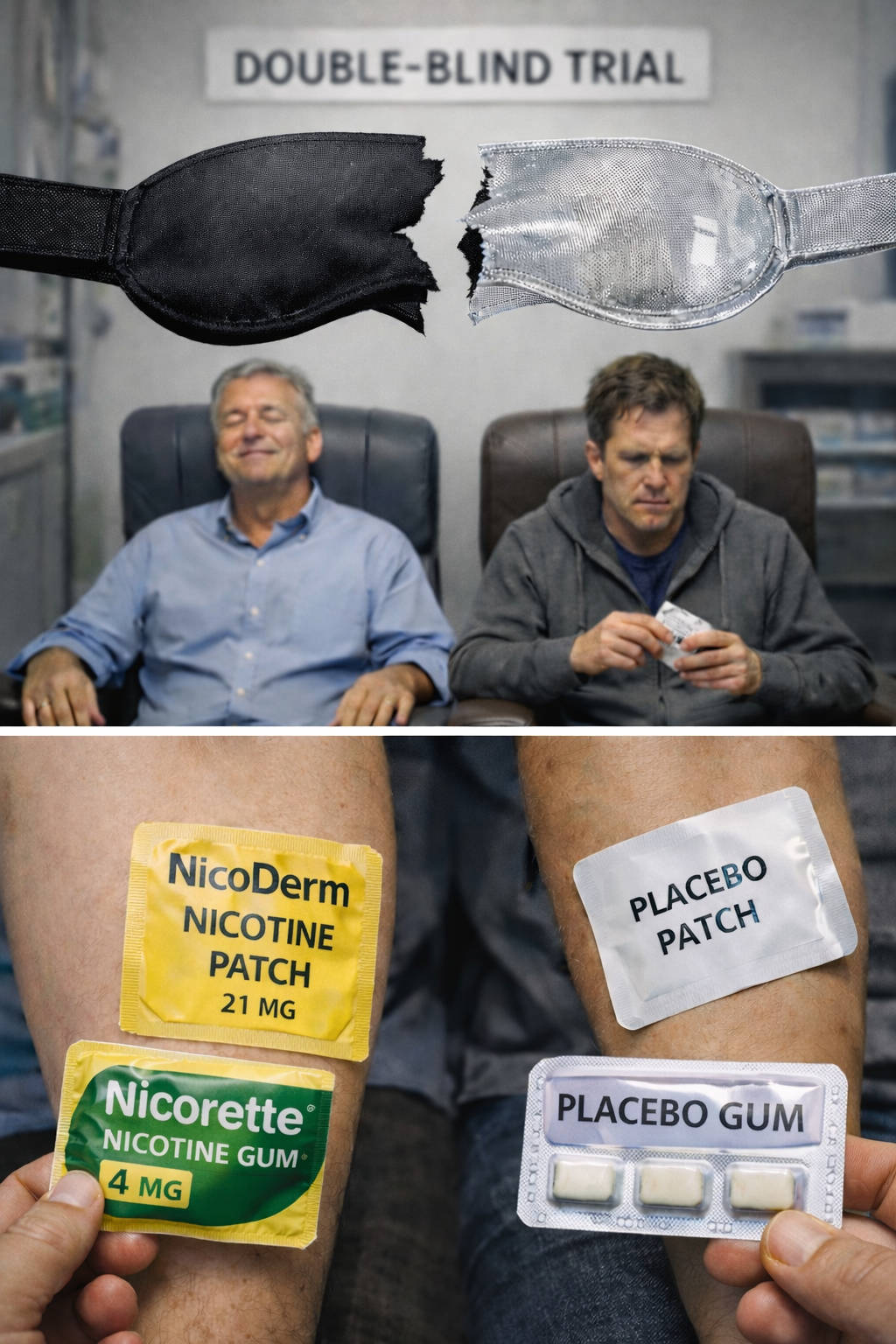
Pretend for a moment that you're still hooked, using, wanting to stop, and curious about NRT but not wanting to spend any money. You hear about a new 4-session nicotine gum stop smoking study at a nearby medical school.
The study is offering a three month's supply of free nicotine gum, counseling, plus travel expense reimbursement. There's only one catch. Half signing up for the study will be randomly assigned to receive nicotine-free placebo gum instead.
Imagine being handed a piece of nicotine gum or a nicotine lozenge while experiencing strong urges to smoke, vape, pouch, dip or chew. How long would it take you to tell whether or not it contained nicotine, or was instead a nicotine-free placebo look-a-like?
Not all of us can do it. The more attempts we've made, the more expert we became at recognizing our withdrawal syndrome.
Still, 3 to 4 times as many of us would be able to correctly say whether we'd been given a placebo, as would declare wrong, and that's within 24-48 hours of attempting to stop (peak withdrawal).[1]
As I wrote in a letter published in the Canadian Medical Association Journal in November 2008, "pharmacologic treatment of chemical dependency may be the only known research area in which blinding is impossible."[2]
We cannot fool cessation savvy nicotine addicts as to whether or not wanting and urges flowing from their brain dopamine pathways have been satisfied.
A June 2004 study was entitled "The blind spot in the nicotine replacement therapy literature: Assessment of the double-blind in clinical trials."[3] It teaches that anyone asserting that NRT studies were blind is not being honest, as far more study participants were able to correctly declare their assignment than couldn't.
Assignment awareness within the active NRT group can be revealed by the fact that nicotine is a psychoactive drug that stimulates the nervous system via the release of adrenaline. This makes the heart pound 10 to 20 beats per minute quicker while elevating blood pressure.
Even more noticeable, nicotine causes the release of dopamine which, at least briefly, satisfies the addict's wanting and desire for more.
Assignment awareness within the study's placebo group (the study's control arm) is even greater than in the NRT group, as their need for nicotine isn't satisfied.
Expecting relief from urges or cravings, the vast majority instead endure their full withdrawal syndrome: a rising tide of anxieties, anger, dysphoria, concentration difficulty, and sleep fragmentation, all within 24 hours of ending nicotine use.
Back to our imaginary study, would you stick around and allow yourself to be toyed with for the next 3 months if convinced that you'd been given placebo gum instead of the real thing? Neither did many of them.
In study after study, 80 to 90 percent of participants reported a history of prior stop smoking attempts. Those attempts taught them to recognize the onset of their withdrawal syndrome. Again, the more prior attempts they'd made, the more expert they became.
But the remaining placebo group members received the exact same counseling, correct? True, but the primary counseling objective in every nicotine replacement study was to foster successful nicotine dependency transfer to an alternative form of delivery, not the lessons and advice needed to minimize the effects of abrupt nicotine cessation (the focus of this book).
If NRT clinical trials were not truly blind, and their outcomes simply reflect fulfilled versus frustrated expectations, what value is there in a study showing twice as many gum users quit compared to those given placebo? Zero.
Imagine the lack of intellectual integrity required to label victory by default - results rooted in frustrated expectations among a group of smokers who went to great lengths to receive free NRT - as having been "science-based."
And this wasn't some old patch-era problem that magically disappeared once newer products arrived. In a 2024 placebo-controlled varenicline trial (generic versions available but marketed as Chantix or Champix prior to June 2021), researchers again found that participants could often discern whether they were receiving the active drug, and that belief about assignment was itself associated with higher quit rates.[8] In other words, expectancy contamination didn't vanish. It followed the industry into its next generation of products.
The placebo story is far more disturbing than time and space permit telling here.
Briefly, ask yourself, who manufactured the placebo devices used in hundreds of trials and who verified their contents? We know that in some trials pharma resorted to putting small amounts of "unbuffered" nicotine into placebo gum and patches. What we don't know is how often "active" placebo use occurred.[4]
Were active placebos spiked with just enough nicotine to keep users in the tease and throes of withdrawal: not delivering enough to satisfy cravings, nor allowing them to get clean, begin re-sensitizing, and move beyond peak withdrawal within 3 days?
The evidence is undisputed and helps explain NRT's real-world ineffectiveness. I wish it wasn't so but, to my mind, declaring clinical trials blind and science-based when they clearly were not, makes pharma nearly as culpable as Big Tobacco in robbing, defeating, and killing smokers.
Falsehood #5: NRT defeated cold turkey in clinical studies
This might surprise you, but those wanting to stop smoking cold turkey have never been invited to compete in clinical trials against self-selecting smokers seeking months of free replacement nicotine, bupropion, or varenicline.[5]
Unlike those going cold turkey, those seeking free "medicine" joined the study in hopes of diminishing their withdrawal syndrome, not quickly meeting, navigating, and moving beyond it.
Again, placebo is not cold turkey. A smoker volunteering for free gum, patches, lozenges, pills, counseling, and travel reimbursement is a different animal from a smoker whose objective is to abruptly end all nicotine use and remain nicotine-free long enough to move beyond peak withdrawal.
Why are there no head-to-head clinical studies pitting "medicine" against cold turkey? Because if honest competition had occurred, NRT, bupropion, and varenicline would have lost, would have never been approved for sale, and there would have been no need for this explanation.
Smoking cessation studies in which the senior researcher has no history of having accepted funding and/or personal payments from the pharmaceutical industry are rare.
Is it reasonable to expect financially conflicted researchers to bite the hand that feeds them? If they did, they know that they'd never receive any pharma money or pharma research project again.
The industry cannot allow its paid army of researchers to conduct intellectually honest studies. They'd cost it billions in lost profits.
It's why smoking cessation clinical trial research is nearly void of scientific integrity. It's why most calling themselves researchers are little more than glorified nicotine salesmen.
We've now seen hundreds of placebo-controlled smoking cessation studies involving NRT, bupropion, varenicline, and now even combination-drug designs, when nearly all agree that placebo affords study participants the worst possible odds of success.[6][10]
But the registry trend is no longer limited to old-fashioned placebo-versus-pill smoking studies. ClinicalTrials.gov now also reflects a gradual shift away from nicotine cessation and toward product switching, nicotine transfer, combination therapies, and harm-reduction studies involving e-cigarettes and nicotine pouches.[11][12][13]
That matters because frustrated cessation researchers are quietly morphing quitting into transfer. More and more, the question is no longer how to help nicotine addicts end dependence, but which product they will switch to, combine, sample, or tolerate. Freedom is quietly being replaced by perpetual dependence.
Switching aside, comparing dependency recovery approaches scientifically is difficult. Randomized trials cannot fairly compare abrupt cessation with drug-seeking volunteers because expectations alone can shape outcomes. The most meaningful comparisons may ultimately come from large population-level observational studies using detailed propensity-score matching to compare real-world recovery paths.
Clinical trial headlines often shout that quitting products “work.” What most smokers don't realize is that these trials rarely test the product alone. Participants typically receive structured counseling, repeated follow-up visits, monitoring, and support that ordinary consumers never receive when they buy the same product at a store or pharmacy.
When a 2018 study examined real-world quitting outcomes using detailed propensity-score matching to compare similar smokers, the expected long-term advantage for pharmaceutical cessation aids largely disappeared.[14] The lesson is simple: in real life, smokers buy the product. They rarely buy the trial.
In other words, the success being promoted may belong partly to the clinical trial environment itself rather than to the product being sold.
Yes, it's fair to add bait and switch to the central abuse. Placebo use continues. But why? Industry research is about the quest for corporate profits and satisfied shareholders. I'm convinced that pharma and the broader nicotine industry are fully aware of the facts I've just shared and intentionally exploit them.
How many participants assigned to placebo in ongoing cessation studies, or steered into transfer studies instead of nicotine freedom, are facing their final confidence opportunity before experiencing a smoking-induced heart attack, stroke, or being diagnosed with terminal cancer or emphysema? What about research ethics?
The current Declaration of Helsinki (compare footnote #7) declares that new interventions should be tested against the best proven intervention, and that placebo or no intervention should be used only for compelling and scientifically sound methodological reasons, with extreme care against abuse.[9] Yet smoking cessation researchers continue sacrificing participants to controls that promise the widest possible margin of victory, the biggest headlines, and the fattest profits.
Also, in pitting cessation products against each other, unless a tie, one product wins and the other loses.
Think about GlaxoSmithKline, maker of Nicorette gum, the Commit nicotine lozenge, the Nicoderm CQ patch, and Zyban. If in GSK's shoes, would you want any of your products to lose to another?
Pharmaceutical companies avoid risk of defeat in head-to-head product competition by use of a control that isn't a real cessation method. That way, no company economic interest gets harmed.
Unfortunately, the lives of clinical trial participants are being sacrificed by a near ethic-less smoking cessation research industry, researchers driven by the quest for personal pharma income, study funding, news headlines, and university tenure.
If this research system seems stacked against nicotine addicts seeking freedom, the next question is obvious: who benefits from it?
References
- 1. Dar R, et al, Assigned versus perceived placebo effects in nicotine replacement therapy for smoking reduction in Swiss smokers, Journal of Consulting and Clinical Psychology, April 2005, Volume 73(2), Pages 350-353 (3.3 times as many correctly determined assignment); also see Rose JE, Precessation treatment with nicotine patch significantly increases abstinence rates relative to conventional treatment, Nicotine & Tobacco Research, June 30, 2009, where 4 times as many placebo patch users correctly determined their placebo assignment as guessed wrong, and did so within one week of quitting.
- 2. Polito JR, Smoking cessation trials, Canadian Medical Association Journal, November 2008, Volume 179, Pages 1037-1038; also see original online e-letter selected for publication, Polito JR, Meta-analysis rooted in expectations not science, E-Letter, Canadian Medical Association Journal, July 17, 2008; and a follow-up e-letter rebutting pharmacology meta-analysis editors' suggestion that blinding issues in drug addiction studies are no different than concerns seen in other studies, Polito JR, Why cessation blinding concerns differ from other clinical trials, E-Letter, Canadian Medical Association Journal, November 9, 2008.
- 3. Mooney M, et al, The blind spot in the nicotine replacement therapy literature: Assessment of the double-blind in clinical trials, Addictive Behaviors, June 2004, Volume 29(4), Pages 673-684.
- 4. Polito JR, FDA knew stop smoking product clinical trials not science-based, Feb. 2, 2019, https://whyquit.com/pr/020219-FDA-knew-stop-smoking-product-clinical-trials-not-science-based.html
- 5. Polito JR, Flawed research equates placebo to cold turkey, WhyQuit.com, March 12, 2007.
- 6. National Institute of Health, www.ClinicalTrials.gov, visited December 2008, search: placebo + smoking.
- 7. World Medical Association, Declaration of Helsinki, Ethical Principles for Medical Research Involving Human Subjects, Adopted by the 18th WMA General Assembly, Helsinki, Finland, June 1964, and last amended by the 59th WMA General Assembly, Seoul, October 2008.
- 8. Schnoll RA, Wileyto EP, Bauer AM, et al. Seeing Through the Blind: Belief About Treatment Randomization and Smoking Cessation Outcome Among People With Current or Past Major Depressive Disorder Who Smoke in a Placebo-Controlled Trial of Varenicline. Nicotine & Tobacco Research. 2024;26(5):597-603. doi:10.1093/ntr/ntad218.
- 9. World Medical Association. Declaration of Helsinki – Ethical Principles for Medical Research Involving Human Participants. Adopted by the 18th WMA General Assembly, Helsinki, Finland, June 1964, and last amended by the 75th WMA General Assembly, Helsinki, Finland, October 2024.
- 10. ClinicalTrials.gov, NCT05206370, A Second Study of Cytisinicline for Smoking Cessation in Adult Smokers, placebo-controlled Phase 3 smoking cessation study, accessed March 11, 2026.
- 11. ClinicalTrials.gov, NCT06218823, Tobacco Treatment Comparison for Cancer Care, active-comparator tobacco treatment study in cancer care, accessed March 11, 2026.
- 12. ClinicalTrials.gov, NCT05327439, Using Pod Based e-Cigarettes and Nicotine Pouches to Reduce Harm for Adults With Low Socioeconomic Status Who Smoke: A Pilot Randomized Controlled Trial, accessed March 11, 2026.
- 13. ClinicalTrials.gov, NCT05715164, Electronic Cigarettes and Nicotine Pouches for Smoking Cessation and Harm Reduction, accessed March 11, 2026.
- 14. Leas EC, Pierce JP, Benmarhnia T, et al. Effectiveness of Pharmaceutical Smoking Cessation Aids in a Nationally Representative Cohort of American Smokers. J Natl Cancer Inst. 2018;110(6):581-587. doi:10.1093/jnci/djx240.